Few conditions are as common, or as commonly misunderstood, as carpal tunnel syndrome. Millions of people live with its hallmark tingling, numbness and nighttime discomfort, yet many wait months or even years before seeking the right care. Understanding what is happening inside your wrist is the first step toward getting better.
This article explains the basics of carpal tunnel syndrome: its symptoms, its causes, how it is diagnosed and most importantly, why a consultation with a hand surgeon is the appropriate starting point for anyone who suspects they may have this condition.
Article Written by
Dr. John M Froelich, MD
Fellowship-Trained Hand & Upper Extremity Surgeon
“The pattern of symptoms, which fingers are affected, when they occur and what makes them better or worse, tells a great deal of the story before a single test is run.”
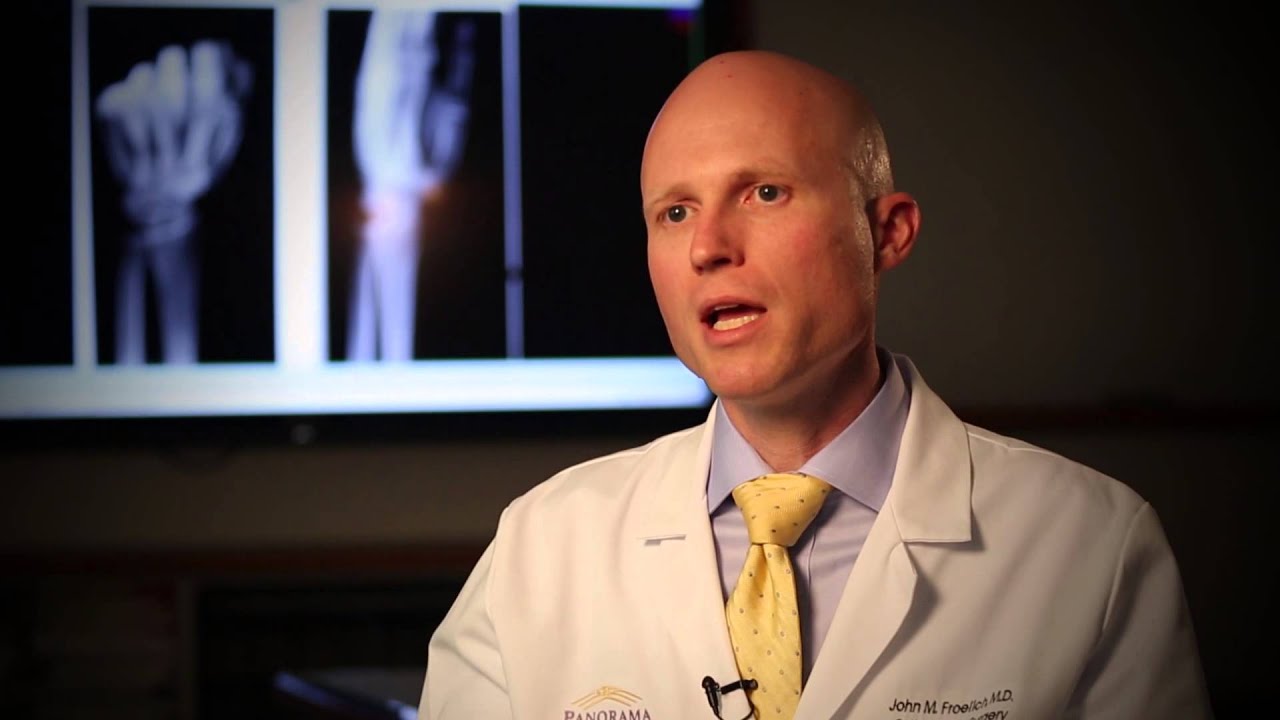
Although carpal tunnel syndrome feels like a very modern ailment, its clinical story stretches back over a century. British surgeon Sir James Paget described compression of the median nerve at the wrist in the 1850s in the context of wrist fractures. However, CTS as a distinct clinical entity was not well characterized until the mid-twentieth century.
In 1950, American neurosurgeon George Phalen published landmark work at the Cleveland Clinic systematically describing the condition and its surgical treatment. [1] His name lives on in the “Phalen’s maneuver,” still used in clinical examination today. Phalen’s surgical series and his advocacy of dividing the transverse carpal ligament to relieve pressure, established the framework for how CTS is understood and treated to this day.
The condition gained enormous public attention in the 1980s and 1990s, when it became associated with computer keyboard use and repetitive assembly-line work. While repetitive motion and prolonged awkward postures can contribute, research has clarified that CTS has multiple causes, including pregnancy, diabetes, thyroid disease, rheumatoid arthritis, obesity and simple anatomy. In many cases, no single cause is identified.
Diagnosis of carpal tunnel syndrome begins with a thorough history and physical examination. A clinician will ask about the pattern, timing and character of symptoms and will perform several specific tests to help identify whether it is carpal tunnel syndrome or something else mimicking the condition.
Durkan’s compression test involves applying direct pressure over the carpal tunnel at the wrist for up to 30 seconds; reproduction of tingling or numbness in the median nerve distribution is a positive result. Durkan’s original research demonstrated this test to have superior sensitivity and specificity compared to other clinical maneuvers. [2, 3] Tinel’s sign refers to tapping over the carpal tunnel at the wrist, a shooting electric sensation into the fingers suggests nerve involvement. Phalen’s test, in which the wrist is held in flexion for 60 seconds, is another commonly used provocative maneuver. Grip and pinch strength may also be measured and sensation carefully assessed.
When clinical findings are uncertain, or when surgery is being considered, electrodiagnostic studies, nerve conduction studies (NCS) and electromyography (EMG), provide objective confirmation. These tests measure how quickly and effectively electrical signals travel through the median nerve, helping quantify the severity of compression and rule out other nerve conditions.
Carpal tunnel syndrome exists on a spectrum from mild to severe, and the best treatment plan depends on where you fall on that spectrum. A hand surgeon, a physician specifically trained in the anatomy, diagnosis and treatment of hand and upper extremity conditions, is uniquely qualified to make that assessment, order the right tests and discuss all options with you honestly. Waiting too long risks permanent nerve damage and muscle loss that may not fully recover even with surgery.
For patients with mild carpal tunnel syndrome, or for those who are not surgical candidates, several non-operative treatments are commonly offered. It is important to understand both what these can achieve and where their limitations lie.
A carpal tunnel splint worn at night to keep the wrist in a neutral position is generally the first treatment option provided. Nighttime splinting can reduce both nighttime and daytime symptoms, even when the splint is not worn during the day. It is low risk, though it does not address the underlying structural problem. For best results, patients should wear the splint consistently for at least four to six weeks before assessing benefit.
Corticosteroid injection into the carpal tunnel can reduce inflammation and swelling around the median nerve, often producing meaningful symptom relief in the short term. Many patients experience significant improvement in the weeks following an injection. However, the evidence for sustained, long-term benefit is limited. [4] A large Cochrane review of multiple research papers on the effectiveness of injections concluded that the short-term benefits of corticosteroid injections do not reliably translate into long-term relief. [6] Injection is best considered a diagnostic tool, a bridge while awaiting surgery or a treatment option for patients with specific reasons to avoid or delay an operation.
Hand therapy and exercise programs, including nerve gliding and tendon gliding exercises and stretching the palm of the hand, are sometimes recommended. These techniques aim to improve the mobility of the median nerve within the carpal tunnel and reduce friction or compression. Some patients find them helpful for temporary symptom management, though these interventions do not traditionally result in long-term relief and are generally more effective in milder cases of carpal tunnel syndrome.
Carpal tunnel release, cutting the transverse carpal ligament to open the carpal tunnel and take pressure off the median nerve, has one of the strongest evidence bases of any elective procedure in hand surgery. When non-surgical treatment options have been exhausted and symptoms persist or worsen, surgery offers a reliable opportunity for lasting relief and prevention of permanent nerve damage.
Carpal tunnel release surgery can be performed with several different techniques, including open, endoscopic and percutaneous approaches. The choice of technique depends on the surgeon’s training and the patient’s anatomy and preferences.
Percutaneous ultrasound-guided thread carpal tunnel release is a newer, minimally invasive option that uses real-time ultrasound imaging to guide a small surgical thread through a tiny skin needle stick to divide the transverse carpal ligament, without a traditional incision. This technique can be performed in the office with only lidocaine for local anesthesia (no heavy medications). Research has shown that patients undergoing thread release experience faster recovery and an earlier return to work compared to those treated with open surgical techniques; one comparative study reported an average return-to-work of 12 days, versus 33 days for open release. [8]
Recovery varies by individual and by technique, but most patients experience significant improvement in numbness and tingling relatively quickly, with strength recovery taking longer. Immediate finger motion is encouraged after surgery. Return to desk work typically occurs within one to two weeks, while manual labor may require four to six weeks. Long-term studies show durable relief in 85-95% of patients at five-year follow-up.
It is important to note that in severe or long-standing cases, complete recovery may not be achievable, another reason early evaluation and carpal tunnel treatment matters. The decision to proceed with surgery is not one to be made lightly, but it is also not one to put off indefinitely if symptoms are progressing. A hand surgeon can help you understand the risks, the expected benefits and the right timing for your specific situation.
Mild or pregnancy-related CTS can sometimes improve once the triggering factor resolves; roughly 90% of pregnancy-related cases improve after delivery. However, most chronic cases do not resolve without some form of treatment and tend to progress over time. Even if symptoms fluctuate, medical evaluation remains important to prevent irreversible nerve damage.
If you have symptoms lasting more than a few weeks, nighttime awakening from numbness or pain, difficulty gripping objects or visible thumb weakness, it is time to see a hand surgeon. Urgent consultation is recommended for sudden severe symptoms, rapidly worsening numbness or signs of another serious nerve or spinal problem.
Carpal tunnel syndrome primarily affects the median nerve and causes numbness, tingling and weakness in specific fingers. Tendonitis involves inflammation of tendons and typically causes localized wrist pain with movement but not true numbness. A careful clinical examination can distinguish these conditions reliably.
Carpal tunnel syndrome is a treatable condition, but treatment works best when it is matched to the right patient at the right time. If you have been experiencing numbness, tingling, dropping items or weakness in your hand, do not dismiss these warning signs.
At Panorama Orthopedics & Spine Center, our hand and upper extremity team includes board-certified hand surgeons who specialize in the full spectrum of carpal tunnel treatment, from splinting and injection to the latest minimally invasive surgical techniques. With same-day and next-day appointments available across six Denver metro locations, getting an expert evaluation has never been more convenient.
Your hands are too important to wait. Schedule an appointment today.