Panorama Orthopedics & Spine Center is the premier foot and ankle care center in Colorado. When it comes to foot and ankle injuries, our experience makes us specially equipped to treat any condition from the toes to the knee, including comprehensive care for both ankles and feet. We address complex foot and ankle deformities, sports injuries, arthritis, cartilage injuries, bunions, and hammertoes. Our team also treats a wide range of disorders, including fractures which can affect the feet and ankles. In addition to sports injuries, we offer specialized sports medicine and rehabilitation services as part of our comprehensive care. For patients needing specialized shoes, we provide guidance on how certain shoe features can influence weight distribution and support for the feet and ankles.
Foot Conditions & Injuries
Our goal at Panorama is to work with you to identify the condition or injury in your foot, so we can help you feel better and do more as quickly as possible.
Big Toe Arthritis
(Joint pain and inflammation)
Bunions
(Bump on toe joint)
Hammer Toe
(Toe deformity)
Midfoot Arthritis
(Joint pain and inflammation)
Subtalar Arthritis
(Joint pain and inflammation)
Neuroma
Plantar Fasciitis
Stress Fractures of the Foot
(Small crack in foot bone)
What is Foot and Ankle Care?
Foot and ankle care is a vital part of maintaining overall health and mobility, as these areas of the body support us through every step of daily life. When foot and ankle conditions arise, whether from injury, chronic disease, or deformity, they can cause significant pain and limit your ability to stay active. That’s why it’s important to seek care from medical professionals who specialize in diagnosing and treating foot and ankle pain.
Their expertise to sports injuries. With advanced skills in both nonsurgical treatments, such as custom braces and specialized shoes, and surgical care, they are equipped to offer the best treatment options for each patient’s unique needs.
Whether you are dealing with a painful acute injury, chronic ankle pain, or a complex disorder affecting the bones, ligaments, or tendons, our specialists are dedicated to providing relief and restoring your mobility. By working closely with patients, orthopedic surgeons develop personalized treatment plans that may include conservative therapies or, when necessary, advanced surgical procedures. Their commitment to excellence in foot and ankle care helps patients return to their daily activities with confidence and comfort.
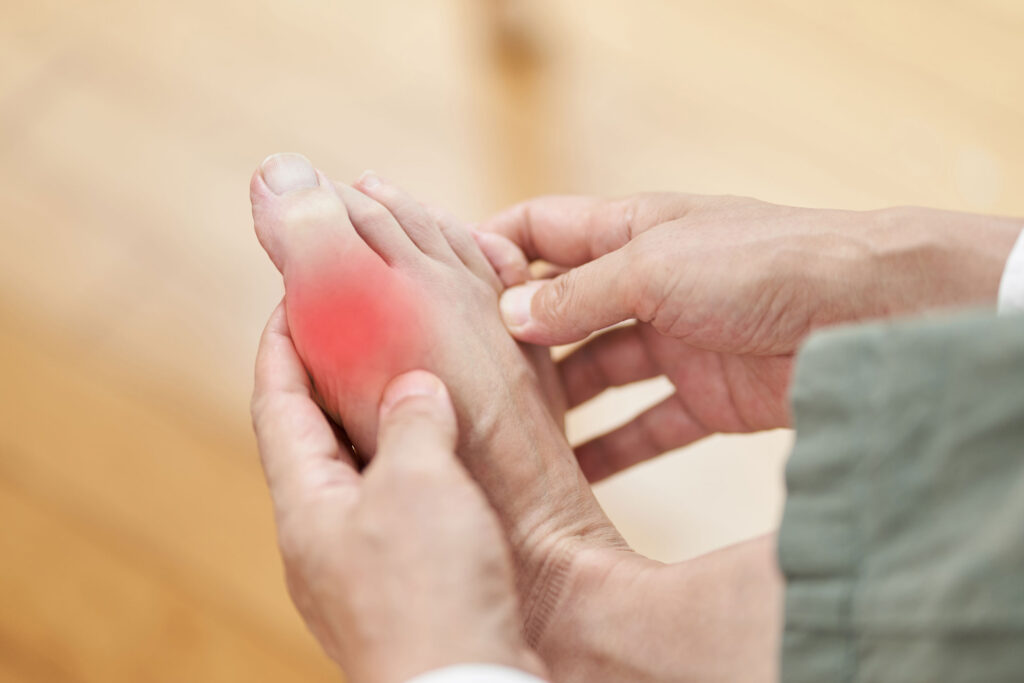
Foot & Ankle Nonsurgical Treatments
If we can, we will always work to avoid surgery by managing foot and ankle conditions through a range of conservative, non-operative treatments, such as bracing, injections, medications, physical therapy and insoles.
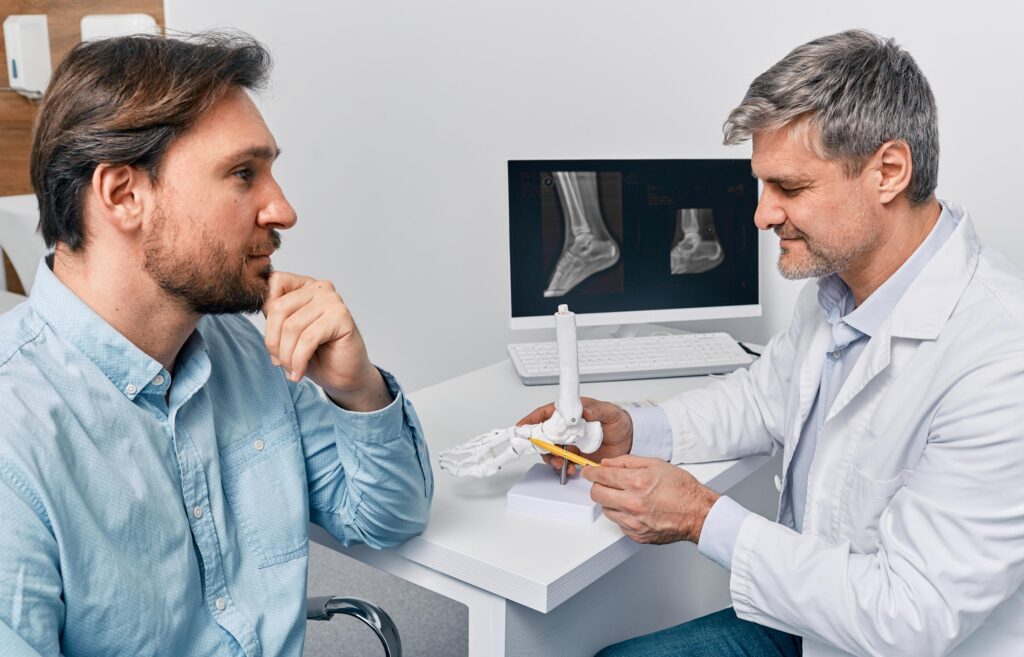
Foot & Ankle Procedures
After our more conservative options have run their course, our experienced team of orthopedic surgeons, specializing in orthopedic surgery, will help you decide the next steps to improve your condition. Some of our surgical options include:
Ankle Fusion
Ankle Fracture Repair Surgery
Big Toe Fusion
Bone Spur Removal
Bunion and Bunionette Repair
Hammer Toe Correction
Ligament Reconstruction
Midfoot Fusion
Tendon Repairs and Transfers
Resources
DOWNLOAD
Lapiplasty® 3D Bunion Correction™ Patient Packet
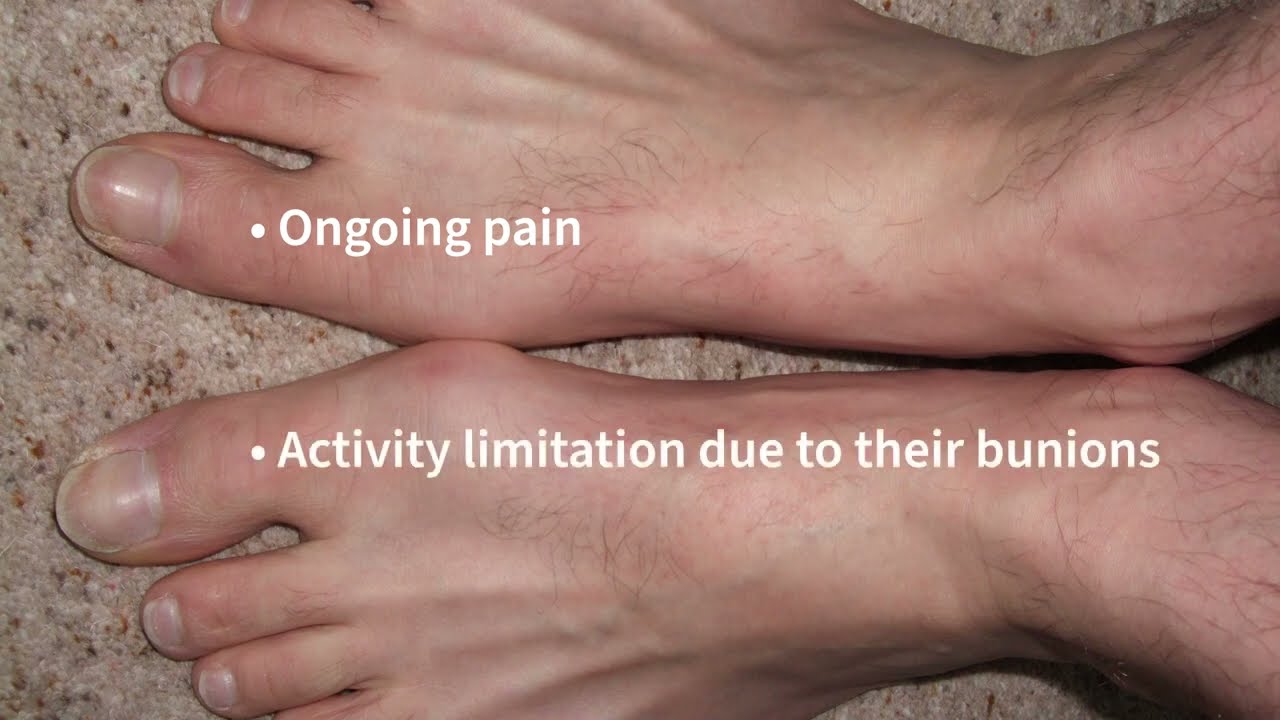
VIDEO
Bunions

VIDEO
Ligament Reconstruction

VIDEO
Ankle Fracture
VIDEO
Achilles Tendon Repair

VIDEO
Total Ankle Replacement

Patient Stories
Jen’s Story
Jen is active and wanted to stay that way! When a bunion on her foot started to restrict her activities, she visited Dr Desai at Panorama Orthopedics & Spine Center for bunion surgery.
